Guide to Cerebral Palsy
» INTRODUCTION TO CEREBRAL PALSY (CP)
» WHAT IS CEREBRAL PALSY?
» WHAT CAUSES CEREBRAL PALSY?
» TYPES OF CP
» TREATMENT AND MANAGEMENT OF CP
» EDUCATIONAL SUPPORTS
» INDEPENDENT LIVING
» AGING AND CP
» MAINTAINING PHYSICAL & MENTAL HEALTH
INTRODUCTION TO CEREBRAL PALSY (CP)
WHAT IS CEREBRAL PALSY?
- CP is a term used to describe a group of disorders affecting body
movement and muscle co-ordination.
- The medical definition of CP is “a non-progressive but not unchanging
disorder of movement and or posture, due to an insult to or anomaly
of the developing brain."
CEREBRAL = OF THE BRAIN
PALSY = LACK OF MUSCLE CONTROL
- Development of the brain starts in early pregnancy and continues
until about the age three. Damage to the brain during this time
may result in CP. This damage interferes with messages from the
brain to the body, and from the body to the brain.
- CP, at its mildest, may result in a slight awkwardness of movement
or hand control. At its most severe, CP may result in virtually
no muscle control, profoundly affecting movement and speech.
Depending on which areas of the brain have been damaged, one
or more of the following may occur:
- Muscle tightness or spasm
- Involuntary movement
- Difficulty with gross motor skills such as walking and running
- Difficulty with fine motor skills such as writing and speaking
- Abnormal perception and sensation
These effects may cause associated problems such as difficulties
in feeding, poor bladder and bowel control, breathing problems,
pressure sores.
The brain damage which caused CP may also lead to other conditions
such as:
- Seizures
- Learning Disabilities
- Hearing Impairment
- Vision Problems
Important notes to remember about CP:
- CP is not contagious
- CP is not hereditary
- CP is not life-threatening
- Limbs affected by CP are not paralysed and can feel pain,
heat, cold and pressure
- Just because someone with CP may not be able to speak or speak
clearly does not mean that they have nothing to say
- The degree of physical disability experienced by a person
with CP is not an indication of their level of intelligence
- People with CP have a normal life-expectancy
- Damage to the brain is a one-time event so the condition will
not get worse although the effects of CP may change overtime
- Some individuals may improve overtime and some may get worse
as tight muscles can cause problems in the hips and spines of
growing children and may require orthopedic surgery; the aging
process can be harder on bodies with abnormal posture or which
have had little exercise.
- It is difficult to estimate exactly how many people have CP.
Many people with mile CP are never diagnosed, while others may
have multiple disabilities which overshadow their CP.
- It is estimated that one out of every 500 babies, and up to
one in three premature babies are affected to some extent. There
are over 50,000 Canadians with CP.
WHAT CAUSES CEREBRAL PALSY?
Any damage to the developing brain, whether caused by genetic or developmental
disorders, injury or disease may produce CP.
During Pregnancy:
Anything, which tends to produce a low birth weight baby, will increase
the likelihood of CP.
Factors during pregnancy which may cause CP include:
- Multiple births (twins or triplets)
- A damaged placenta which may interfere with fetal growth
- Infections
- Poor nutrition
- Exposure to toxic substances, including nicotine and alcohol
- Maternal diabetes, hyperthyroidism or high blood pressure
- Premature dilation of the cervix leading to premature delivery
- Biochemical genetic disorder
- Chance malformations of the developing
During labour:
- Premature delivery
- Abnormal positioning of the baby (such as breech or transverse
lie) which makes delivery difficult
- Rupture of the amniotic membranes leading to fetal infection
In early childhood:
CP can occur if a young child suffers brain damage due to:
- Infections such as meningitis
- Brain hemorrhages
- Head injury following falls, car accidents or abuse
- A lack of oxygen (asphyxia) due to accidents such as drowning
- Seizures
Not many years ago, CP was usually described as being caused
by "a lack of oxygen at birth". Researchers have come
to realise that the causes are far more complex. In many cases,
a difficult labour may be a symptom rather than a casue of CP.
Many people with CP are born prematurely, but other families sail
through a straightforward pregnancy and deliver to be hit by CP
"out of the blue".
Every person with CP asks "why did this happen to me?"
and every parent of a child with CP asks "did I do anything
wrong?". In most instances, these questions will never be
answered to your satisfaction. As one mother said, "When
I stopped saying 'why me?' I was ready to accept my son's CP and
look to the future."
Diagnosis of CP
- CAT (Computerized Axial Tomography) and MRI (Magnetic Resonance
Imaging) can identify lesions in the brain. This technology enables
some children who are considered at risk of having CP to be diagnosed
very early
- For the majority of people with CP it will be months or sometimes
years before a diagnosis is confirmed
- A child with CP will probably be delayed in reaching their ”milestones”
such as rolling over, sitting and standing
- A baby may feel unusually stiff or floppy
- A diagnosis of CP is unlikely to be given until the child’s progress
is observed over a period of time and other conditions are ruled
out
TYPES OF CP
- With so many different causes of CP, it is no surprise that it
takes many forms. Every person with CP is a unique individual, but
is likely to be classified as having a particular type of CP.
- Classification can be according to the type of movement disorder
and/ or by the number of limbs affected
Classification by Number of Limbs Involved
 Quadriplegia
- All four limbs are involved
Quadriplegia
- All four limbs are involved
 Diplegia -
All four limbs are involved. Both legs are more severely affected
than the arms
Diplegia -
All four limbs are involved. Both legs are more severely affected
than the arms
 Hemiplegia
- One side of the body is affected. The arm is usually more involved
than the leg.
Hemiplegia
- One side of the body is affected. The arm is usually more involved
than the leg.
 Triplegia
- Three limbs are involved, usually both arms and a leg.
Triplegia
- Three limbs are involved, usually both arms and a leg.
 Monoplegia
- Only one limb is affected, usually an arm.
Monoplegia
- Only one limb is affected, usually an arm.
Classification by Movement Disorder
The location of the brain injury will determine how movement
is affected.
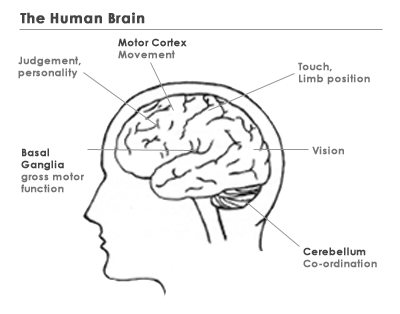
Spastic CP
Spastic CP is the most common type and is caused by damage to the
motor cortex. Spastic muscles are tight and stiff, which limit movement.
Normal muscles work in pairs, when one group contracts, the other
group relaxes to allow free movement in the desired direction. Spastic
muscles become active together and block effective movement. This
muscular tug-of-war is called co-contraction.
Spasticity may be very mild and affect only a few movements, or
very severe and affect the whole body. The amount of spasticity
usually changes over time.
Choreo-Athetoid CP
Choreo-Athetoid CP results from damage to the basal ganglia or cerebellum
and leads to difficulty in controlling and co-ordinating movement.
Children may have involuntary movements (which frequently cease
while they sleep), or have difficulty with skills that require coordinated
movements such as speech or reaching and grasping objects smoothly.
Some terms commonly used to describe these involuntary movements
include:
Athetosis – slow, writhing movements, particularly in the hands
and face
Ataxia – unsteady walking and balance problems, Ataxia results
from damage to the cerebellum, the brain’s major center for balance
Chorea – jerky movements of the head, arms or legs
Dystonia – twisting movements and postures of the trunk or limbs
Mixed-type CP
When areas of the brain affecting both muscle tone and voluntary movement
are affected, a diagnosis of Mixed-Type CP may be given. Usually the
spasticity is more obvious at first, with involuntary movement increasing
as the child develops.
The classifications of movement disorder and number of limbs involved
are usually combined (e.g. spastic diplegia). These technical words
can be useful in describing the type and extent of CP, but they are
only labels. A label does not describe an individual.
TREATMENT AND MANAGEMENT OF CP
CP is not considered to be a curable condition and the word “management”
is used more often than “treatment”. However, there is much that can
be done to lessen the effects of CP and to help people with CP to
lead independent lives.
If you have a child with CP it is easy to be overshelmed by the number
of professionals involved with your child and the different management
and therapy options. Not all interventions are appropriate for each
individual and, as a parent, you are the person to decide what is
right for you and yor child. Some parents like to involve their child
in every option that may be helpful; others decide that having family
time is more important than spending hours each week on therapy or
the stress involved in going through another bout of surgery. Some
adults with CP consdier the therapy and/or surgery they had as children
was very helpful; others quit therapy in adolescence and stay as far
away from doctors and therapists as they can.
Therapy
- Physical Therapy (PT) aims to help people achieve their potential
for physical independence and mobility. PT includes exercises, correct
positioning and teaching alternate ways of movement such as walkers,
bracing or handling a wheelchair.
- Occupational Therapy (OT) designs purposeful activities to increase
independence through fine motor skills. OTs help children to use
adaptive equipment such as feeding, seating and bathroom aids.
- Speech Therapy aims at improving communication. A child may only
need help to overcome a slight articulation problem, or she may
not be able to communicate verbally and may require a non-verbal
communication system. Alternate communication systems can include
synthesized and natural spech devices.
- Music Therapy uses music for the treatment of neurological, mental
or behavioural disorders.
- New therapies are being developed all the time. Contact your local
Cerebral Palsy Association for information on alternative treatments.
Orthotics, Casts, and Splints
Most children with CP will be prescribed orthotics, casts or splints
to supplement their therapy programs. These should be custom made
for the child and help to provide stability, keep joints in position,
and help stretch muscles.
Medications
A child may take medication for conditions associated with their CP,
such as seizures. Drugs may sometimes be prescribed for severe spasticity
or painful spasms. Spasticity can be reduced by nerve blocking injections.
A recent development is the infection of botulinum toxin ("Botox")
into a spastic musle group. This can reduce tone for several months.
Surgery
- Orthopaedic and soft-tissue surgery can help to counter the damaging
effects of spasticiy on the spine, hips and legs. Surgery can lengthen
or transfer tendons, enabling the child to move more easily. When
the child has finished growing, bone surgery may help to reposition
and stabilize bones.
- Neurosurgery involves surgery on the nerve roots which control
muscle tone. Selective posterior rhizotomy aims to reduce spasticity
by severing some of the nerve roots in the spine.
Adaptive Equipment
An enormous range of aids and adaptive equipment are now available
for people with disabilities. As the number of elderly people in Canada
increases, more daily living aids are coming onto the market.
Mobility Devices include:
- wheelchairs (manual, power and sports)
- scooters
- specially made bicycles and tricylces
- walkers and crutches
Communication Devices include:
- symbol boards
- voice synthesizers
- head sticks and keyguards for computers
Daily Living Aids include:
- electronic door openers
- large-handled eating utensils
- grab sticks
- environmental control systems
Some equipment is availble through provincial health and social service
systems. These vary across the country. Your local Cerebral Palsy
Association can advise you what is available in your area.
EDUCATIONAL SUPPORTS
Many children with CP will also have some type of learning disability.
Assessment by a psychologist, and the support of special educators
can reduce the handicapping effects of a learning disability.
Canada has some of the world's best "early intervention"
programs. Children with CP will often start their education early
to help improve their mobility and communication skills before starting
school.
Most children with CP will receive an integrated education enabling
them to mix with their peers in their neighbourhood school. A child
with mild CP may simply require minor program adjustments. For example,
he may need a little more time to write an exam if his hand control
is poor. A child with more severe disabilities may require considerable
support from resource staff and teaching assistants.
Children should have an Individualized Education Plan (I.E.P.) which
assesses the child's performance, sets goals and specifies which supports
are required. The amount of support offered, and the commitment to
successful integration, varies widely between school boards and individual
schools. A good partnership between parents and educators will help
achieve their goals.
'The ultimate long-term goal is realistic
independence. To get there we have to have some short-term goals,
those being a working communication system, education to his
potential, computer skills and, above all, friends'. - Parent
of boy with CP
INDEPENDENT LIVING
The efects of CP are lessened considerably by an environment that
enables people with disabilities to play a full part in their communities.
It is never too early to start working toward future independence.
Barriers for people with disabilities, both physical and attitudinal,
have lessened due to the efforts of disability groups and the support
of social policy-makers. There is still much to do, but Canada can
take pride in being one of the worlds most progressive countries on
disability issues
People with cerebral palsy can live independently
and be productive members of the workforce.
Living with CP
A person with CP has to cope both with disabilities and handicaps.
A disability is a physical loss of function such as being unable to
walk, having difficulty with hand control or speech. A handicap is
the degree to which that disability puts you at a disadvantage in
daily life. Fore instance, someone who is very short-sighted may be
considered to have a disabilitiy, but she is unlikely to consider
this a handicap if she has corrective lenses. A disability may prevent
someone with CP from climbing stairs, but this will only be a handicap
if the building whe wants to enter is not wheelchair-accessible. CP
is not a life-threatening condition and, in itself, is no barrier
to leading a long and produ tive life. People with CP enjoy satisfying
careers, university education, social life, and become parents. Some
limitiation are unavoidable, but very few people manage to achieve
their dreams of becoming olympic athletes, concert pianists or brain
surgeons.
The key elements to minimizing the handicapping effects of CP are:
Management and Treatment
Therapy, surger and the use of adaptive equipment help many people
with CP to use their minds and bodies to their full potential.
Access
You cannot lead an idependent life if public buildings, washrooms
and transportation are not accessible. To have a good career you
need educational opportunities. To have a satisfying social life
you need acccess to recreational facilities and opportunities to
develop friendships.
Attitudes
It is very hurtful to have someone pat you on the head if you are
sitting in a wheelchiar, or to walk away because they cannot understand
what you are trying to say to them. Prejudice and teasing can be
very damaging. A good sense of self-esteem is required to cope with
these negative attitudes. Children can also be handicapped if they
are over-protected and allowed to become too dependent. People with
disabilites are people first and should never be described by such
negative labels as 'wheelchair-bound', 'spastic', or 'afflicted
with cerebral palsy'. All people share similar needs, desires, drives
and responsibilities.
AGING AND CP
- It is hard to generalize about how CP affects aging.
- Although people with CP are considered to have a normal life expectancy,
the physical challenges of CP may intensify with age (such as increased
spasticity, fatigue, loss of strength and declining mobility).
- A decline in mobility may be due to weight gain, lack of therapy
and exercise, and the development of other conditions such as arthritis.
- These physical challenges can in turn lead to increased stress
and anxiety.
- A positive attitude makes a big difference, and developing relaxation
techniques and coping skills have a beneficial effect on mental
and physical heath.
- It can be frustrating for adults to deal with a health care system
that appears to have little knowledge or interest regarding the
changing needs of aging with a disability. A positive attitude makes
a big difference, and developing relaxation techniques and coping
skills can have a beneficial effect on mental and physical health.
MAINTAINING PHYSICAL & MENTAL HEALTH
A lifestyle that involves regular exercise and proper nutrition is
important for everyone, including those with disabilities. A good
general fitness level will help with range of motion and flexibility.
Exercise to improve cardiovascular fitness can improve endurance and
help offset age-related changes that lead to fatigue. A nutritious,
high-fibre, low-fat diet will help avoid problems with constipation
and weight gain and will increase energy levels.
Having CP does not make you immune to other condititions. People
with CP are as likely as anyone else to contract heart disease, cancer
or diabetes. Sometimes a change in the body can be put down to an
effect of CP when it is actually a different condition.
The 1990s has seen a shift to a wellness concept of health care with
emphasis on self-directed care that requires the individual to take
responsibility for decisions and actions that affect their overall
health. Individuals need appropriate knowledge, attitudes and skills
to make these decisions. Learning strategies to increase independence
and develop coping skills is a life-long process. Parents can foster
attitudes that promote self-sufficiency and build self-esteem. Adults
with disabilities need to learn to take an active role in their personal
health management.
The importance of learning skills to increase independence and self-confidence
throughout an individual's lifetime cannot be over-empasized. The
stresses associated with aging will be lessened if a person is able
to maintain a postivie personal attitude, if he is involved in meaningful
activities, and if he has developed a supportive environment. He needs
confidence to seek information, to plan for age-related changes, and
to be an active participant in his healthcare and lifestyle choices.